Many therapists believe that having a “normal” spinal curve is associated with less or no back pain. Thus, people with too much or too little lordosis are at a higher risk of getting low back pain. However, much of the research in the past 20-plus years do not support such causative relationship.
In fact, a recent systematic review and meta-analysis published in The Spine Journal seem to support the idea that the lack of lumbar lordotic curve angle is indicative of low back pain — that is, IF you only glance at the abstract. Researchers from Seoul, South Korea, reviewed 13 studies — which were only observational studies such as cohort, case-control, and cross-sectional — that totaled almost 800 low back pain subjects and 927 healthy controls. When the data are pooled together, they found that those with low back pain have a lower lordotic curve than those with no low back pain. (1) While this is generally what the researchers concluded, there is more to the story.
Lordosis research on back pain
Although a majority of the studies (n=9) found a strong relationship between a lordotic curve and low back pain, the researchers also found other potential contributors to pain, including disc degeneration, spinal stenosis, disc herniation, and other spinal diseases. Other factors that increase the likelihood of having low back pain include age, gender, pain severity and chronicity, and the nature of the spinal disease. For example, lumbar lordosis tends to decrease with age, women seem to experience more low back pain than men, and disc herniation often is associated with in a lower lordotic curve.
However, the researchers cannot find any significant association from these factors they were examining due to the mixed methods and interpretations of the included studies. “While a significant association between attenuated lumbar lordosis and low back pain was evidenced by the results of this meta-analysis, no causal relationships were able to be surmised based on the data from observational studies,” they wrote.
Some of the limitations in this review include high heterogeneity among the studies (65%), low quality assessment of the risk of bias, lack of control for factors that might affect the lordotic curve, lack of reporting of blinding of the evaluator, and exclusion of spondylolisthesis because many studies excluded this disease.
Lordosis and back pain: correlation does not imply causation
We can see why it is easy to jump to conclusions and say that the lumbar spine curvature is a cause of low back pain based on this review, but a closer examination reveals that it isn’t so. Chun et al. cautioned about their findings because previous systematic reviews and larger, higher quality studies find that there spinal curvature plays a very minor role in determining low back pain.
An Australian review and meta-analysis published in BMC Musculoskeletal Disorders found hardly any differences in low back pain between those higher or lower lordotic curve. (3) However, Chun et al. stated, “…the heterogeneity among studies included in this meta-analysis seems to have been underestimated. [This] review dealt with studies that employed clinical measures, while radiologic methods are more suitable for measuring the absolute parameters of [lumbar lordotic curve].” (1)
Another study from Quebec published in European Spine Journal found that asymptomatic subjects had high variability in the sagittal alignment of the spine, and the researchers stated that examining the lordotic curve cannot determine whether someone has low back pain or not. (2)
Lordosis as an adaptation or response to pain
It is likely that changes in posture and how people move are ways they adapt to avoid pain. Moseley and Hodges investigated this and found that there was a delay in muscle activation during the pain trials, and these muscles return to their normal state during the no pain trials. “The results suggest that altered postural adjustments of the trunk muscles during pain are not caused by pain interference but are likely to reflect development and adoption of an alternate postural adjustment strategy, which may serve to limit the amplitude and velocity of trunk excursion caused by arm movement,” they concluded. (4)
Another study from Aalborg University in Denmark suggested that pain reduces stability and increased postural changes, such as having larger sway during a balance test. Pain also made the subjects take longer time to return to their balanced and stable state while standing on a movable platform, which could increase their likelihood to fall. (5)
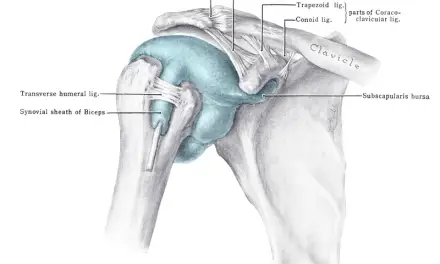
Among subjects with hunched shoulders, recent research find that this may be an adaptation to avoid shoulder impingement syndrome that is caused by compression between the coracoacromial arch and the humerus during shoulder elevation above the shoulder height. (6)
Looking these findings, it is possible that a reduction of lumbar lordosis— in some cases — an adaptation to pain, whether it stems from disc degeneration or a fear-avoidance behavior. (7) While Chun et al. admits that there is a dearth of good data on this subject, ignoring the relevance of the lumbar lordosis among low back pain patients is not good practice. Likewise, putting too much emphasis on posture can also be problematic since it may cause a nocebic response to patients. (8)
So look at the bigger picture than just zeroing on a piece of flesh or bone. Your patients or clients could tell you more than just your observations.
References
1. Chun SW, Lim CY, Kim K, Hwang J, Chung SG. The relationships between low back pain and lumbar lordosis: a systematic review and meta-analysis. Spine J. 2017 May 2. pii: S1529-9430(17)30191-2. doi: 10.1016/j.spinee.2017.04.034.
2. Chaléat-Valayer E, Mac-Thiong J-M, Paquet J, Berthonnaud E, Siani F, Roussouly P. Sagittal spino-pelvic alignment in chronic low back pain. European Spine Journal. 2011;20(Suppl 5):634-640. doi:10.1007/s00586-011-1931-2.
3. Laird RA, Gilbert J, Kent P, Keating JL. Comparing lumbo-pelvic kinematics in people with and without back pain: a systematic review and meta-analysis. BMC Musculoskeletal Disorders. 2014;15:229. doi:10.1186/1471-2474-15-229.
4. Moseley GL, Hodges PW. Are the changes in postural control associated with low back pain caused by pain interference? Clin J Pain. 2005 Jul-Aug;21(4):323-9.
5. Hirata RP1, Ervilha UF, Arendt-Nielsen L, Graven-Nielsen T. Experimental muscle pain challenges the postural stability during quiet stance and unexpected posture perturbation. J Pain. 2011 Aug;12(8):911-9. doi: 10.1016/j.jpain.2011.02.356.
6. 1. Muraki T, Yamamoto N, Sperling JW, Steinmann SP, Cofield RH, An KN. The effect of scapular position on subacromial contact behavior: a cadaver study. J Shoulder Elbow Surg. 2017 Jan 11. pii: S1058-2746(16)30540-7. doi: 10.1016/j.jse.2016.10.009.
7. Gatchel RJ, Neblett R, Kishino N, Ray CT. Fear-Avoidance Beliefs and Chronic Pain. J Orthop Sports Phys Ther. 2016 Feb;46(2):38-43. doi: 10.2519/jospt.2016.0601.
8. Darlow B, Dowell A, Baxter GD, Mathieson F, Perry M, Dean S. The Enduring Impact of What Clinicians Say to People With Low Back Pain. Annals of Family Medicine. 2013;11(6):527-534. doi:10.1370/afm.1518.
A native of San Diego for nearly 40 years, Nick Ng is an editor of Massage & Fitness Magazine, an online publication for manual therapists and the public who want to explore the science behind touch, pain, and exercise, and how to apply that in their hands-on practice or daily lives.
An alumni from San Diego State University with a B.A. in Graphic Communications, Nick also completed his massage therapy training at International Professional School of Bodywork in San Diego in 2014.
When he is not writing or reading, you would likely find him weightlifting at the gym, salsa dancing, or exploring new areas to walk and eat around Southern California.