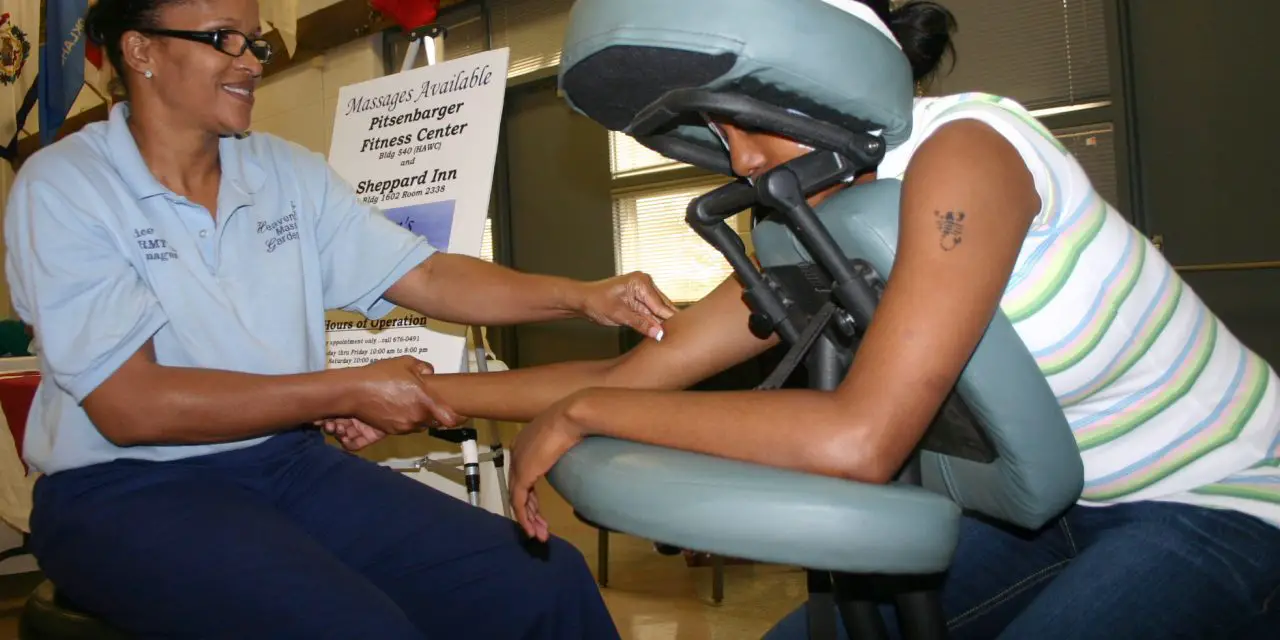
Massage therapy can help alleviate anxiety and depression symptoms among veterans and refugees, but is the profession ready to care for this population?
“Ever since my wife died, I can’t sleep—the back pain keeps me awake all night,” said the patient who was a Vietnamese refugee who had served in the South Vietnamese military during the Vietnam War in the 1970s. He came to the United States when South Vietnam was defeated. His physician, who had prescribed painkillers and anti-depressants to break the pain cycle, referred him for massage therapy. Psychological evaluation had yielded various diagnostic terms, including “somatization,” but that offered no relief of symptoms or distress for him.
If this man sought you for help in your practice, what would you do for him?
If you have ever felt like you were punched in the gut when you heard bad news, or you have struggled to catch your breath when someone rejected you, then you already understand what the term “somatization” means. Psychiatrist Zbigniew J. Lipowski defined somatization as “a tendency to experience and communicate somatic (bodily) distress in response to psychosocial stress, and to seek medical help for it.” It refers to pain or other symptoms that are medically unexplained after biological causes for the symptoms have been tested and ruled out.
In some circles, the word “somatization” is considered highly problematic because it can have connotations of hypochondriasis or attention-seeking, implying that the person who reports symptoms is faking or their problem is “all in their head.” At worst, the term is seen as a form of victim-blaming. These connotations are not what we mean. We are referring to a physical suffering that clients seek massage and other treatments for to get relief. If we keep our focus on our clients’ real suffering, then the term itself is less important than the actions that we take in response to that suffering.
There is a great deal that we do not yet know about how the process of somatization translates psychosocial distress into physical symptoms. We do know that it represents a massive problem in economic, medical, and social terms worldwide.
Management is expensive and difficult because these symptoms are persistent. They lead to suffering and frustration for the patient because many treatments are ineffective in addressing the symptoms. The patients’ distress persists, despite adhering to what their healthcare practitioners advise them to do.
Clinicians also tend to find this inability to help relieve patients’ suffering frustrating. Sometimes they react to this frustration by prescribing multiple medications in the hope that something might work, or by handing off the patients to other practitioners. For these reasons, prevention is far preferable to management after symptoms appear, but the sociopolitical and cultural obstacles to prevention are formidable because they involve addressing issues of equity and change in core economic, political, and social structures.
Emotional Expressions Between the East and West
In my experience providing massage therapy, veterans and refugees have a particularly large burden of medically unexplained physical symptoms that they live with daily. Many of them came from Southeast Asia, including a large population of Vietnamese who came to the United States after the Vietnam War. Vietnamese culture has traditionally drawn on Chinese culture for centuries and has taken many ideas from China and transformed them into a particularly Vietnamese take on them. One idea that radiated from China into other cultures that it influenced was the idea that love and other emotions are not normatively spoken or demonstrated.
For example, rather than saying “I love you” as someone might do in the U.S. or Europe, you demonstrate your love by the act of commitment to going to work everyday to provide for their well-being.
People from Chinese-influenced cultures feel emotions as strongly as anyone else does. However, the emotions that are the most motivated for them may not be the ones that are most motivated for people from other cultures. Anthropologist Robert Levy drew an important distinction among “hypercognized” and “hypocognized” emotions within particular cultures.
“Hypercognized” emotions are those that are designated as appropriate to speak about with one another. Similarly, “hypocognized” emotions are designated as unimportant, not worth discussing, and not of interest. The social norms of particular cultures may de-emphasize talking with others about certain emotions or even about emotional life in general.
When people from these cultures find themselves resettled as refugees, and they seek medical help for symptoms, sometimes they find a clash between their expectations for treatment and the recommendations that the medical system offers them, especially if their provider recommends the unfamiliar mode of talk therapy for what their own culture has designated as appropriately hypocognized.
For example, in a particular refugee culture, patriotism may be hypercognized, and individual ambition is hypocognized. One of the refugees, who was a former literature professor, said how disappointed and depressed he is to be unemployed here since did not speak English. The youths, who would have held him in high esteem back home, disrespected him and does not want to learn the old language and literature. He is also actively discouraged from expressing those feelings to others. So he spends his days playing mah-jong and watching TV programs he does not understand. He goes to the clinic to see me for massage therapy so he can sleep better.
Another refugee sought massage therapy for pain from an injury he incurred while impressed into a militia to fight the government (without pay), while his family waited for him for several years in a refugee camp in a nearby country. When one of the (now Americanized) children criticized the militia that forced him to fight, he reacted angrily to the suggestion that his patriotism might be misplaced, and the expatriate culture approved of that angry reaction. Understanding the relationships among the situations, the emotions, and the experienced pain or insomnia is not easy or obvious for either of these patients.
In the military culture, talking about your feelings to others is not always encouraged. The military has a job to do, and that mission is paramount, even if lives have to be sacrificed to accomplish it. Individual emotions and self-expression are not part of that mission. They are hypocognized in military culture. “Suck it up and drive on” is an informal service motto, and that means that military often work through serious injuries, underreport them, and continue to live with the after-effects rather than feel that they are letting down their unit by taking time out to seek treatment. Someone with a mild or moderate brain injury from combat, for example, may refuse treatment on the spot (when it has the potential to be more effective) in order to stay with the unit. Thus, the symptoms become more deeply established.
This approach of “suck it up and drive on” often persists, even after they have left the military and returned to civilian life. This attitude, which can be very different from civilian behavioral expectations, can create a formidable barrier between the veteran and loved ones, employers, and other civilians.
Many of the extreme stressors veterans and refugees encounter can be very similar — war, witnessing death of loved ones, serious injury, and other physical and emotional trauma. They find themselves in situations that provoke intense emotions.
It can be obvious to see how this can be a strong social pressure that encourages somatization. Physical complaints are taken seriously by others in a way that emotional ones often are not, even in societies that are relatively open in discussing emotions. It does not mean that they are faking it, or that the symptoms are “all in their head.” The distress resulting from what they have experienced is real and justified, and the outlets for seeking care for that distress are influenced and shaped by interactions among the biology of our nervous system, the psychology of the affected individual, and the larger society’s cultural expectations of appropriate illness and wellness behaviors.

Photo: Unknown. Source: U.S. Marines in Japan Homepage
Massage Therapy, Anxiety, Evidence
Many veterans and refugees who came to see me primarily for pain: headaches, back pain, abdominal pain, and sleeping difficulty. Often left unspoken is the effect that anxiety, depression, and other psychological symptoms are having on their quality of life because seeking massage therapy for a physical complaint is more socially tenable than psychological complaints. However, research had demonstrated that massage therapy can alleviate symptoms of anxiety:
“Quantitative research reviews show that a series of massage therapy treatments consistently produces sizable reductions of depression in adult recipients. The effects of massage therapy on anxiety are even better understood. Single sessions of massage therapy significantly reduce state anxiety, the momentary emotional experiences of apprehension, tension, and worry in both adults and in children, and multiple sessions of massage therapy, performed over a period of days or weeks, significantly reduce trait anxiety, the normally stable individual tendency to experience anxiety states, to an impressive degree in adults.
“Together, these effects on anxiety and depression are the most well-established effects in the massage therapy research literature. They are especially important for us to understand not only for their own sake, but also because anxiety and depression exacerbate many other specific health problems. In other words, it is reasonable to theorize that quite a few specific health benefits associated with massage therapy may actually be ‘second-order’ effects that are a consequence of massage therapy’s ‘first-order’ effects on anxiety and depression. For all these reasons, the anxiety- and depression-reducing effects of massage therapy can form the basis of new testable theories that will guide future research and help to determine how, when, and for whom massage therapy works. ~ Dr. Christopher Moyer (1)
Consistent with Moyer’s interpretation, veterans and refugees alike report that massage therapy is effective for treating pain and sleep difficulties. It is highly plausible that these reported second-order effects not only reflect first-order improvements in their anxiety and depression, but they can serve as a bridge to making science-based psychological treatments (such as cognitive behavioral therapy) directly targeted at anxiety and depression—a more acceptable alternative for consideration than they first appear to the client. Being part of a health care team at a major medical center makes responsibility, communication, and treatment modifications like these much easier than does the relative isolation of private practice, compounded by an outsider status.
Massage Therapy as Part of a Health Care Team
Massage therapy needs to be ready to commit to being part of an entire patient-centered professional healthcare team to be able to serve this population better. This commitment means accepting mainstream health care professional ethical values and knowledge. It means committing to remain within our scope of practice, even if we feel like we understand psychology. It means working with a team, and with supervision, to ensure the safety of vulnerable and at-risk patients.
It means accepting reality because our clients do not have the luxury of rejecting that reality, and we stand with them in facing it. For the client whose story began this article, reality meant mixed results. My team and I did not completely relieve his insomnia, but we were able to co-create a massage routine that reliably provided him four to five nights of quality sleep between our weekly appointments. He was satisfied with those results, and we continued them for several years.
Right now, even if we were willing as a group to make that commitment, we are not adequately prepared to do so. Unlike the members of the current professional health care team, we do not even have an undergraduate level preparation for practice, much less the graduate-level education and discernment that they bring to the treatment encounter. Our curriculum does not prepare us for the reality of practice among clients with complex and multifactorial conditions, such as medically-unexplained physical pain compounded by anxiety and depression, and further complicated by low socioeconomic status and readjustment difficulties.
We have to replace those outdated concepts about how our body and mind work with the understanding of biopsychosocial issues to provide service to clients living with complex and pervasive conditions. Knowing Levy’s distinction between hypercognized and hypocognized emotions, for example, prepares us far better to provide effective massage for someone from a refugee or military culture than belief in a non-existent human energy field ever will.
We have a great deal of preparation and hard work ahead of us if we want to faithfully serve these clients. If we are willing to commit to that mission, then we also have much to offer to them and to their quality of everyday life.
Taking Moyer’s challenge to actively develop an “affective massage therapy” discipline opens up a world of possibility for the development of our profession through a better understanding and application of massage therapy’s real-life mechanisms. This improves the health and well-being of all of our clients by addressing underlying conditions that complicate the physical experience of suffering.
Reference
1. Moyer C. Affective Massage Therapy. Int J Ther Massage Bodywork. 2008; 1(2): 3–5.