Examining the evidence behind treatments for depression and pain and massage therapists’ scope of practice when working with patients with such symptoms.
During the Christmas season of 2014, Andrew Jones, who is a registered massage therapist (RMT) working at Massage Now in London, Ontario, Canada, was waiting for his mother to pick him up from the airport at Regina, Saskatchewan. His mom arrived, picked him up, and they headed home via the highway. Minutes later, a drug-impaired driver veered into their lane head-on and collided into his family’s ’97 Ford Taurus at the left headlight, sending the vehicle spinning into a ditch facing the highway.
“That saved us from any further impact from the vehicles following us, screeching and crashing into Mister Meth’s offending vehicle [that was] already flipped upside-down,” Andrew told me in an online interview, “The impaired driver walked away with minor head injuries. The driver behind us hurt his knees. I got whiplash and nearly broke my left arm and was obviously traumatized. I was cut up a bit too.”
His mother, however, was not so fortunate. After Andrew got his bearings, he looked around and saw that she was unconscious, slumped over the steering wheel. Terror swamped over him, but he kept his wits and called 911.
“Once I knew help was on its way, I started screaming at my mom to wake up. She came to and I kept speaking to her making sure she didn’t fall unconscious. She kept drifting in and out of consciousness. People came over, telling me help was on its way. I remember someone giving me a bottle of water, trying to help. I didn’t drink it since I had no idea if I had internal injuries.
“The ambulance came, then the firefighters. Mom was pinned in the vehicle. She had a traumatic brain injury with a shattered jaw. Broken clavicle. Left humerus broken radially and distally. Open compound fracture of the left radius and ulna both proximally and distally. So were her left femur, tibia and fibula and foot and ankle. Her right foot was broken as well. She spent three long months in the hospital. She is amazing and is up and walking. Her left arm was saved and she had an incredible surgeon.”
The near-death experience triggered pain from post-traumatic stress disorder (PTSD) in Andrew, who had it from a childhood trauma. Events like this affect him daily, which lapses Andrew in bouts of deep depression. “I am generally in fight or flight mode, so I try and turn that over-amped mentality and hyper-vigilance into a hyper-focus and analytical mindset,” Andrew said, who currently suffers from chronic neck and sacroiliac joint pain. “Physical pain accompanied most of these events, but I feel pretty guilty complaining considering the agony my mother experienced.
“I am so glad I still have my mom.”
When pain strikes with depression
While traumatic events such as the one Andrew had experienced can trigger symptoms depression, anxiety, or other disorders, subtle stimuli — such as a song played at a mall, the smell of a specific perfume, or a color and pattern of a shirt — could also trigger such symptoms that could last for many months and years. These symptoms include uncontrolled crying, melancholy that “paralyzes” the body, inability to find pleasure in things that were once enjoyable, and shunning social contact.
Pain is also another common symptom that accompanies depression and anxiety. In many ways, such pain is similar to physical pain, and it can be difficult to determine whether someone has mostly physical or emotional pain at first because the symptoms are often similar. Some studies have shown that physical pain (e.g. temperature) and emotional pain (e.g. rejection) “light up” similar parts of the brain that process pain, such as the anterior dorsal cingulate and anterior insula.(1,2)
However, a 2014 study published in Nature Communications show otherwise, stating that shared activities do not necessarily correlate to shared processes of pain. Physical pain and emotional pain process differently on a micro-level. (3)
While research continues to unravel the mechanisms behind pain and cause-and-effect relationship, the latest definition of pain encompasses cognition and social influences with sensory and emotional factors. (4)
People suffering from pain and depression experience physical pain that are often similar to those with the same physical pain (e.g. back pain, headaches) but without depression. Thus, depression is not just a psychological disorder when other factors, such as relationships and environment, also influence it.
This brings a question to many researchers and clinicians: Which causes the other: depression or pain?
What does the evidence say about depression and pain?
While the research and scientific evidence about the association between depression and pain are mixed and somewhat inconclusive, most find a connection between these two conditions. One recent Australian systematic review published in The Spine Journal found that the evidence on the symptoms of depression as a prognostic factor for low back pain is inconsistent — based on 17 studies in which 13 of them are cohort studies — but the entire evidence generally points to an association between the two. (5)
Researchers from the University of Sydney, lead by Dr. Marina Pinheiro, found that studies that found no association between depression and pain have small sample sizes, However, four studies with large sample sizes suggested the contrary.
“The study that found the strongest association between depression and low back pain divided participants as having or not severe symptoms of depression and used compensation status as outcome measure. It is possible that symptoms of depression may have higher impact in the prognosis of low back pain in people with more severe levels of low back pain, such as patients with compensation claims,” the researchers stated. (5)
Likewise, symptoms of depression could increase the chances the getting new episodes of low back pain, according to another systematic review published Arthritis Care & Research in 2016. Based on 11 qualified studies with over 23,000 participants, older people are more likely to have another bout of low back pain with depression, which further debilitate and increase the risk of having pain and/or depression. (6)
Pinheiro et al. cautioned that we should not extrapolate these recent findings as a causation of pain or depression since there are many underpinnings of low back pain and depression that are not entirely understood. Biological links between depression and pain is plausible since they share common biological pathways. (8) Deficiency of neurotransmitters could affect positive moods and emotions and lower pain thresholds. Also, those who are less physically active, have less social interactions, or have sleep disorders are more susceptible to depression and pain. (6)
Research in depression’s association with neck pain and knee pain yield similar results yet psychosocial factors are still a portion of the bigger picture. (7,9,10)
Treatments for depression and pain
Treatment for depression and pain vary among individuals. While some people may be able to overcome and manage depression and pain on their own, many people will need therapeutic treatments and coping skills as well as social support. Rather than choosing a treatment that is “popular” or based on a single or a few “it-works-for-me” stories, clinicians, patients, and clients should examine the current evidence and reasoning behind different treatments. However, it does not mean that we should discount anecdotes; instead, we should use them as a start of an investigation of a treatment’s effectiveness, not a conclusion.
For Andrew, cognitive behavioral therapy (CBT) helped him “to keep in check,” but that treatment alone probably would not have helped him manage his pain and depression well.
“I cope using medication, CBT techniques, massage therapy, meditation, working out, and Brazilian jiu-jitsu,” he said. “I also play my guitar, have an amazing girlfriend, and have two kitties to cheer me up.”
Psychosocial treatment
Some people going through depression may relate to what Andrew is going through with his treatment and management, but some may not know what CBT is.
“Cognitive behavioural therapy is a form of psychological therapy often used to treat mental health problems, but also used to help people make changes in health beliefs and behaviours. It employs the underlying conceptual models used in cognitive behavioural therapy, but it is a broader approach that can be adopted by many different health professions,” Dr. Bronnie Thompson explained to me in an online interview, who teaches at the Department of Orthopaedic Surgery and Musculoskeletal Medicine at the University of Otago Christchurch Health Sciences in New Zealand.
“In a cognitive behavioral approach the person is encouraged to reconceptualise their pain as something to be managed rather than necessarily abolished. People can learn different ways of coping with their pain and living as normal a life as possible. They can also develop an approach to ‘living well’ that reduces their focus on waiting for a cure and returns the focus on personal-relevant goals.”
The current Cochrane Review on the efficacy of psychological therapy (e.g. CBT) via the internet with pain reduction is somewhat promising, but further research is still needed because of a low number of high-quality trials and mixed results from different studies.
However, with depression and anxiety, the results are not so promising. The authors concluded:
“Internet-delivered cognitive behavioural therapy (CBT) for the management of chronic pain in adults may be effective for the short-term management of pain, disability, depression, and anxiety in individuals with chronic non-headache pain conditions, but there is currently limited evidence for their effectiveness for headache pain and disability, and no evidence for their effectiveness on depression and anxiety in individuals with chronic headache conditions. On average, participants entering trials of Internet-delivered treatment are mildly disabled and distressed. No conclusions can be made for treatments other than CBT. We do not know if these treatments are associated with adverse events and we do not know how satisfied participants are with these treatments.”
They also “do not know what can work for whom and in what context” since research on this topic is still in its early stages of development.
The gray drizzle of horror induced by depression takes on the quality of physical pain. But it is not an immediately identifiable pain, like that of a broken limb. It may be more accurate to say that despair, owing to some evil trick played upon the sick brain by the inhabiting psyche, comes to resemble the diabolical discomfort of being imprisoned in a fiercely overheated room. And because no breeze stirs this caldron, because there is no escape from this smothering confinement, it is entirely natural that the victim begins to think ceaselessly of oblivion. ~ William Styron (1925-2006)
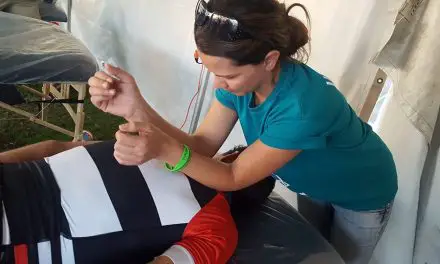
Effects of caring touch
It is no surprise to many people that massage therapy can reduce pain and could alleviate symptoms of depression. While research on this specific topic is scant, there is some scientific evidence that massage therapy can be a qualified and adjunct treatment for patients with clinical depression. In a 2004 meta-analysis of massage therapy for various conditions — including depresion and anxiety — researchers from the University of Illinois Urbana–Champaign found that participants had more than 77 percent trait anxiety reduction than comparison group participants. Likewise, those with depression had more than 73 prcent reduction of the symptoms than its comparison group participants.
The researchers also compared the effects of massage therapy to that of psychotherapy, the latter in which is a more traditional treatment for anxiety and depression. In some ways, the two professions are similar in explaining why some patients feel better after a treatment. One theory proposed is that the effects of massage therapy has little to do with the treatment or technique itself, but rather the patient’s expectations of the treatment’s outcome, the warm, friendly personality of the therapist, and the interaction between the therapist and the patient. These factors are independent of the therapist’s skill level and training of massage.
So far, little is known and certain about the physiological and psychological outcomes of massage therapy because there has been very few updates and higher quality research on massage effects on depression and pain since the 2004 meta-analysis.
However, the positive outcomes of massage therapy on depression may likely be a combination of physiological and psychological factors that research have yet to tap in.
“The best currently available evidence indicates that the effect of MT [massage therapy] on stress hormones is weak. This finding is surprising, given the strong effects of MT on anxiety and depression, because those conditions are known to be linked with changes in endocrine system activity,” wrote Dr. Christopher Moyer in “Affective Massage Therapy.”
“Why has a strong MT effect on stress hormones not been uncovered? One possibility is that there is a strong stress hormone effect that can result from MT, but that the effect occurs only under certain conditions that have not yet been delineated in the research. If this is the case, such an effect could be “washed out” when average effects are calculated across subjects within a specific study, or across studies in research reviews.
“Another possibility that must be considered is that any endocrine changes that result from MT are not themselves the cause of reductions of anxiety and depression, but merely an imperfect indicator that such reductions have occurred by another mechanism. If this is the case, it would explain why MT effects on anxiety and depression are consistently larger than MT effects on stress hormones.” (18)
Pain is part of the human experience. As is suffering. Unfortunately, we will likely need to live with pain and persevere through suffering. It does not need to be disabling and functionality can be restored. Suffering can be lessened, but many times pain will still follow you like Churchill’s black dog of depression. ~ Kevin Holmes, PT
Exercise for depression and pain: mixed results but promising
“¡Wepa!”
I have been dancing salsa since the summer of 2002. Even now, dancing was an adjunct to my existing physical activity during my post-college years, which was weight-lifting. I was already taking hip-hop and breakdancing lessons at the time for about two years, but I gradually transitioned to the social Latin dance in 2003. The euphoria I experienced during salsa that I experienced back then still exists today. Perhaps this is one primary reason why many people go social dancing — the music, the movement, and the touch you give and receive to other people. Sometimes I feel reluctant to leave, especially when there are many great dancers and the DJ plays several sets of songs that draw you back to the dance floor.
Salsa — or almost any social dancing in general — is no longer just a leisure activity. While some people certainly feel more like laughing than breaking into tears for no apparent reason after a workout or dancing for three hours, the evidence behind the efficacy of exercise in reducing the symptoms of depression is mixed — yet promising.
The most recent Cochrane Review found — based on 39 studies with a total of over 2,000 subjects — exercise to be “moderately more effective than a control intervention for reducing symptoms of depression,” but most of the studies’ methodology quality was low. Exercise appeared to be no more effective than psychological or pharmacological therapies, the researchers concluded. (13)
Likewise, for children and adults suffering from depression after a traumatic brain injury, the quality of evidence for exercise to treat depression is very low due to poor methodology and lack of quality randomized-controlled trials.14 However, three other systematic reviews have slightly different results. (15,16,17) While one review concluded that methodology in most qualified studies were low and the results are mixed, exercise as an effective treatment for depression “may be a ‘gold bullet,’ considering the low cost, the benefits on global health, and the acceptable risk.” Even though the researchers were somewhat optimistic about the results, they cautioned that recommending exercise instead of usual care may be hazardous because of the “continuing ambiguous evidences of findings on the topic.” Yet there are some evidence that exercise, when combined with antidepressants, may be beneficial initially during treatment. (15)
Another review from the University of Cumbria in the U.K., had a more positive viewpoint on the effects of exercise on mild depression. Based on 13 qualified trials, exercise seems to be effective when combined with psychotherapy or medication, and exercise should be the “first-line treatment” for mild depression under the The National Institute for Health and Care Excellence guidelines. Like the previous reviews mentioned, the author agreed that the methodologies are poor, “if methods are refined, as advised, significant findings could emerge that impact mental health policy.” (16)
Respecting scope of practice while caring for those with depression and pain
Sometimes we massage therapists can step beyond our scope of practice and boundaries to play psychotherapist or counselor when dealing with clients who have symptoms of depression. While the U.S. lacks a coherent scope of practice for massage therapists in regards to what they may or may not do legally, two common grounds are soft tissue manipulation and such manipulation should have a therapeutic intent or purpose.
“Beyond these two major points, legislative and professional discrepancy begins,” Christy Cael wrote in the September/October 2009 issue of Massage & Bodywork. (19)
Although some massage schools in the U.S. teach students to recommend exercises for clients, some states may exclude exercise recommendation within the scope of practice.
“Be particularly mindful not to assign any numbers to suggested movements (i.e., do this stretch three times a day and hold for 30 seconds each time); that is clearly exercise prescription and the territory of physicians, exercise physiologists, physical therapists, and fitness professionals,” Cael wrote.
“When in doubt, refer out.”
Canada, however, is a different world. Lee Kalpin, a RMT and massage educator in Ontario, Canada, told me online that their scope of practice is pretty straight-forward.
The Massage Therapy Act of 1991 in Ontario states, “The practice of Massage Therapy is the assessment of the soft tissue and joints of the body and the treatment and prevention of physical dysfunction and pain of the soft tissue and joints by manipulation to develop, maintain, rehabilitate or augment physical function, or relieve pain.” (20)
If a patient has depression, RMTs stick with treating the muscles and other soft tissues. “If a client’s depression is causing symptoms that affect the muscles etc, we can treat that. We are not treating the ‘depression’ itself, but the side-effects of depression,” Kalpin explained.
“If a person has symptoms of depression, come to me for treatment of neck pain and headaches, then that would be the major focus of my treatment — the neck pain and headaches. We always interview, assess and suggest a treatment plan. If the patient agrees to that plan, then that is our focus of treatment.”
RMTs in British Columbia also has very similar scope of practice and approach. “We do recommend exercise and are encouraged to by our regulator,” Michael Roech, RMT, told me in an online interview, who is a member of Registered Massage Therapists Association of British Columbia (RMTBC) and lobbies for their scope of practice. “If I suspect depression, I’ll administer an evidenced-based questionnaire and send the results to their physician to interpret. We can treat the soft tissue symptoms of the patient or as directed by their physician.”
Working with the clinically depressed can be quite challenging, considering the complexity behind the problem, treatments, evidence, interaction, and scope of practice that are different in different countries. If massage therapy is to be recognized as part of a healthcare team to help treat those with chronic pain and mental issues, then we need to have a common ground in identifying our scope of practice, education, and ethics.
As our understanding of pain and depression improves, our way of thinking and explaining what we do with our hands and our interaction with our clients and patients need to change accordingly.
Patients and clients with depression should not be deterred from receiving quality massage therapy. Even if the effects of the treatment is likely to be transient, a few extra nights of quality sleep or having higher motivation to exercise and be more social could have longer-term effects.
“Don’t give up. There is always hope. There is always the possibility things will get better, even in the worst of times,” Andrew added. “I know the pain can seem unbearable, but continue to search for the treatment that will work for you.”
References
1. Eisenberger NI, Lieberman MD, Williams KD. Does rejection hurt? An FMRI study of social exclusion. Science. 2003 Oct 10;302(5643):290-2.
2. Kross E. et al. Social rejection shares somatosensory representations with physical pain. Proc Natl Acad Sci U S A. 2011 Apr 12;108(15):6270-5. doi: 10.1073/pnas.1102693108.
3. Woo C W. et al. Separate neural representations for physical pain and social rejection. Nature Communications. 2014 Nov 17; 5 (5380): doi:10.1038/ncomms6380
4. Willaims CDC A., Craig K. Updating the definition of pain. Pain. 2016 May 18.
5. Pinheiro MB1, Ferreira ML2, et al. Symptoms of depression as a prognostic factor for low back pain: a systematic review. Spine J. 2016 Jan 1;16(1):105-16. doi: 10.1016/j.spinee.2015.10.037.
6. Pinheiro MB1, Ferreira ML2 et al. Symptoms of Depression and Risk of New Episodes of Low Back Pain: A Systematic Review and Meta-Analysis. Arthritis Care Res (Hoboken). 2015 Nov;67(11):1591-603. doi: 10.1002/acr.22619.
7. Schere M., Blozik E., et al. Depression and anxiety as major determinants of neck pain: a cross-sectional study in general practice. BMC Musculoskelet Disord. 2009; 10: 13. doi: 10.1186/1471-2474-10-13
8. Bair MJ, Robinson RL, Katon W, Kroenke K. Depression and pain comorbidity: a literature review. Arch Intern Med 2003; 163:2433–45.
9. Linton SJ. A review of psychological risk factors in back and neck pain. Spine 2000;25:1148–56.
10. Cicuttini FM et al Are depression, anxiety and poor mental health risk factors for knee pain? A systematic review. BMC Musculoskelet Disord. 2014;15:10. doi: 10.1186/1471-2474-15-10
11. Eccleston C1, Fisher E, Craig L, Duggan GB, Rosser BA, Keogh E. Psychological therapies (Internet-delivered) for the management of chronic pain in adults. Cochrane Database Syst Rev. 2014 Feb 26;(2):CD010152. doi: 10.1002/14651858.CD010152.pub2.
12. Moyer CA1, Rounds J, Hannum JW. A meta-analysis of massage therapy research. Psychol Bull. 2004 Jan;130(1):3-18.
13. Rimer J1, Dwan K, Lawlor DA, Greig CA, McMurdo M, Morley W, Mead GE. Exercise for Depression. Cochrane Database Syst Rev. 2012 Jul 11;(7):CD004366. doi: 10.1002/14651858.CD004366.pub5.
14. Gertler P, Tate RL, Cameron ID. Non‐drug treatments for depression in children and adults who have had a traumatic brain injury. Cochrane Database of Systematic Reviews 2015, Issue 12. Art. No.: CD009871. DOI: 10.1002/14651858.CD009871.pub2.
15. Mura G, Sancassiani F, Machado S, Carta1 MG (2014) Efficacy of Exercise on Depression: A Systematic Review. International Journal of Psychosocial Rehabilitation. Vol 18(2) 23-36
16. Webster L. The effectiveness of physical activity as an intervention in the treatment of depression: A systematic review. Journal of Applied Psychology and Social Sciences, 1 (1) 28-40.
17. Josefsson T1, Lindwall M, Archer T. Physical exercise intervention in depressive disorders: meta-analysis and systematic review. Scand J Med Sci Sports. 2014 Apr;24(2):259-72. doi: 10.1111/sms.12050. Epub 2013 Jan 30.
18. Moyer C. Affective Massage Therapy. Int J Ther Massage Bodywork. 2008; 1(2): 3–5.
19. Cael C. Scope of Practice. Massage & Bodywork Magazine. 2009 Sept/Oct.
20. Massage Therapy Act, 1991, S.O. 1991, c. 27. Government of Ontario.
A native of San Diego for nearly 40 years, Nick Ng is an editor of Massage & Fitness Magazine, an online publication for manual therapists and the public who want to explore the science behind touch, pain, and exercise, and how to apply that in their hands-on practice or daily lives.
An alumni from San Diego State University with a B.A. in Graphic Communications, Nick also completed his massage therapy training at International Professional School of Bodywork in San Diego in 2014.
When he is not writing or reading, you would likely find him weightlifting at the gym, salsa dancing, or exploring new areas to walk and eat around Southern California.