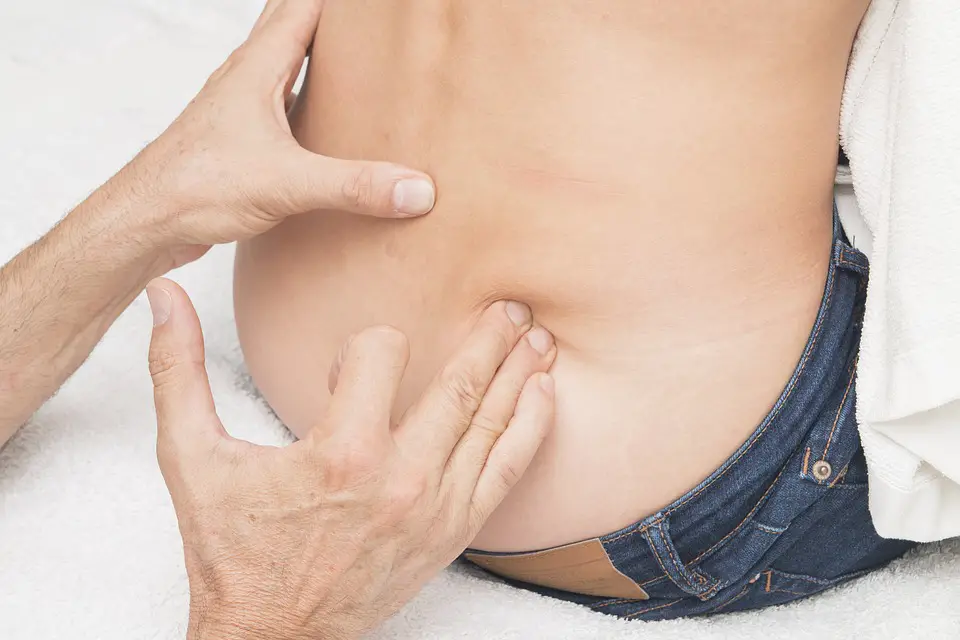
Pelvic tilt ‘corrections’ are still a big hype in manual therapy and fitness professions, yet recent research finds a lack of evidence that it needs correcting for back pain.
If a physical therapist or personal trainer had told you that have an anterior pelvic tilt and you need treatments to “correct” it, chances are, you should get a second opinion. A recent systematic review finds a lack of evidence that some non-surgical treatments are effective in reducing excessive anterior pelvic tilt and “potentially related symptoms.” (1)
Researchers from Odense University Hospital in Denmark, led by Dr. Anders Brekke, leafed through more than 5,000 citations in various databases that fit their research criteria, which includes absence of disease and non-pregnant subjects. There was no language restriction in their search. They funneled down to four papers: two randomized-controlled trials (RCTs) and two non-randomized trials. (2, 3, 4, 5)
Each of these trials have different treatments, including Rolfing (2), sacroiliac joint adjustment with hip stretches (3), abdominal strengthening exercises (5), and taping (4). Although some of these studies show a reduction of low back pain (2,3,4) and decreased anterior pelvic tilts, Brekke at al. find them to have high risks of bias because of a lack of blinding of the therapist, assessors, and subjects and missing reports on how the subjects were randomized. (2,5)
While there is lack of quality evidence that having an anterior or posterior pelvic tilt is a strong cause or has a strong association with back or hip pain, this research indicates that even such interventions, like massage and exercise, has little to no benefits in addressing the pelvic tilt. Brekke et al. suggests that there should be further investigation of “high-quality interventions targeting non-surgical treatment as an alternative to invasive surgery in reducing anterior pelvic tilt….”
They also said that there is no evidence that support the idea that anterior pelvic tilts is an “isolated clinical disorder or pathology.” Establishing a cut-off point for an excessive anterior pelvic tilt can be a problem because of individual variability in anatomy and movement where each person has their own way of maintaining balance and movement efficiency. There is no cookie-cutter factor that regulates each person’s movement and posture. (9)
Should anyone try to correct an anterior pelvic tilt?
Based on the current scientific literature, probably not. If you can move well, go to work without (much) pain, and engage in your favorite activities regularly with your anterior pelvic tilt, you may be just fine. If you do have back pain, there may be other reasons why pain persists. The broad scientific literature on posture and structural “abnormalities” in relation to back pain and various musculoskeletal pain often show a lack of strong correlation and causality between both factors.
For example, an early study from California State University Long Beach in 1990 found “No correlation was found to exist between hip extension [range of motion], standing pelvic tilt, standing lumbar lordosis, and the double leg-lowering abdominal muscle performance test” among 25 healthy, pain-free subjects. (6)
A large 2002 study of 600 people in Tehran, Iran, found that structural factors, such as pelvic tilt, the degree of lumbar lordosis, and length of abdominal and psoas muscles, “are not associated with the occurrence of [low back pain].” (7) People with or without low back pain had variations of pelvic tilts that make identifying who has back pain or not challenging for clinicians.
Even a systematic review of 43 studies fails to find pelvic tilts as a reliable predictor and indicator of people having low back pain. However, the researchers do find that those with low back pain tend to walk and bend forward slower than those without pain, and they are more likely to have lower proproception in “repositioning” to neutral position after they perform a trunk flexions and extensions. (8)
Remember that pain is more than just about a “misaligned” piece of anatomy or tissue damage. Your anterior pelvic tilt may just be a small piece of the bigger puzzle of pain—or not at all.
References
1. Falk Brekke A, Overgaard S, Hróbjartsson A, Holsgaard-Larsen A. Non-surgical interventions for excessive anterior pelvic tilt in symptomatic and non-symptomatic adults: a systematic review. EFORT Open Rev. 2020;5(1):37–45. Published 2020 Jan 29. doi:10.1302/2058-5241.5.190017
2. Cottingham JT, Porges SW, Richmond K. Shifts in pelvic inclination angle and parasympathetic tone produced by Rolfing soft tissue manipulation. Phys Ther. 1988 Sep;68(9):1364-70.
3. Barbosa AC, Martins FL, Barbosa MC, Dos Santos RT. Manipulation and selective exercises decrease pelvic anteversion and low-back pain: a pilot study. J Back Musculoskelet Rehabil. 2013;26(1):33-6. doi: 10.3233/BMR-2012-0347.
4. Lee JH, Yoo WG, Kim MH, Oh JS, Lee KS, Han JT. Effect of posterior pelvic tilt taping in women with sacroiliac joint pain during active straight leg raising who habitually wore high-heeled shoes: a preliminary study. J Manipulative Physiol Ther. 2014 May;37(4):260-8. doi: 10.1016/j.jmpt.2014.01.005. Epub 2014 Apr 26.
5. Levine D, Walker JR, Tillman LJ. The effect of abdominal muscle strengthening on pelvic tilt and lumbar lordosis. Physiother Theory Pract 1997;13:217–226
6. Heino JG, Godges JJ, Carter CL. Relationship between Hip Extension Range of Motion and Postural Alignment. J Orthop Sports Phys Ther. 1990;12(6):243-7.
7. Nourbakhsh MR, Arab AM. Relationship between mechanical factors and incidence of low back pain. J Orthop Sports Phys Ther. 2002 Sep;32(9):447-60.
8. Laird RA, Gilbert J, Kent P, Keating JL. Comparing lumbo-pelvic kinematics in people with and without back pain: a systematic review and meta-analysis. BMC Musculoskelet Disord. 2014;15:229. 2014 Jul 10. doi:10.1186/1471-2474-15-229.
9. Roussouly P, Gollogly S, Berthonnaud E, Dimnet J. Classification of the normal variation in the sagittal alignment of the human lumbar spine and pelvis in the standing position. Spine (Phila Pa 1976). 2005 Feb 1;30(3):346-53.
A native of San Diego for nearly 40 years, Nick Ng is an editor of Massage & Fitness Magazine, an online publication for manual therapists and the public who want to explore the science behind touch, pain, and exercise, and how to apply that in their hands-on practice or daily lives.
An alumni from San Diego State University with a B.A. in Graphic Communications, Nick also completed his massage therapy training at International Professional School of Bodywork in San Diego in 2014.
When he is not writing or reading, you would likely find him weightlifting at the gym, salsa dancing, or exploring new areas to walk and eat around Southern California.